
Toward Reliable Healthcare Systems
The covid-19 pandemic has wiped out decades worth of global health progress. This has affected different countries disproportionately, as weaker healthcare systems were more prone to the pandemic. While service coverage has improved in the last 20 years, the proportion of people facing financial hardship due to out-of-pocket health spending has increased. With rising poverty and shrinking incomes resulting from the global economic recession and health systems struggling to provide continuity of health services, the COVID-19 pandemic is likely to halt the progress made towards universal health coverage, particularly among disadvantaged populations. Even amongst nations with powerful economies and high GDP like the United States, performance of their medical sector was subpar at combatting the covid pandemic. The resulting average cumulative deaths due to covid of a US state are between 100-130% higher than that of a European country. If one lesson can be taken from the preventable loss of life that was witnessed on an unprecedented scale in modern history, it is that strengthening the healthcare systems of countries should become a top priority.
Many differing health systems are utilized around the world currently. What constitutes a strong, reliable healthcare system? If that can be identified, we can create a model to serve as the ideal that healthcare sectors on a worldwide scale should strive for.
The differing relevant predictors are as follows:
- Expenditure on health sector
- Source of funding (Government or private funding)

- Allocation of funds
The following data reflects the relevant metrics between the years 2012 and 2020. The USA is a clear outlier when it comes to the spending budget in their health sector, in terms of both Government and private spending, totaling $10,921 spent per capita. The East Asia & Pacific, as well as the Middle-East, are on the other side of the spectrum, with very low funding from all sources at an average of $742 and $507 per capita respectively. As for the European union, its spending is somewhere in between, at an average of $3476 per capita.
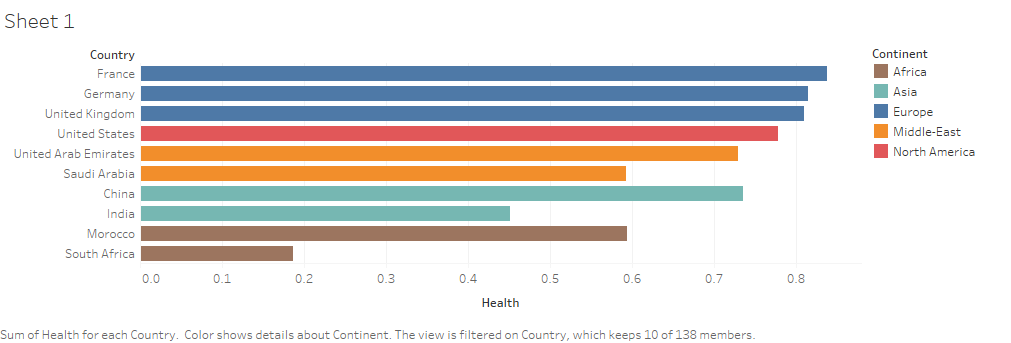
For our determinant of healthcare performance, the utilized metric we will use is the health indicators published by the WDI in 2019. Despite the USA’s excessive healthcare expenditures, it still scores lower than the European countries on health indicators. Despite the low spending in China, Saudi Arabia and the United Arab Emirates, they both command strong health metrics. India and Morocco on the other hand, despite spending less than South Africa, still have significantly higher health metrics.
This is to show that spending budgets do not correlate to the performance of a health sector. Instead, allocation of the funds seems to be the more deterministic variable, as all the countries of the European union, as well as the UAE, Saudi Arabia, and China have Universal healthcare or a system that closely resembles it at the very least. Despite lower levels of spending, the precise designation of these funds has led to significantly higher health indicators. In addition, systems that adopt universal healthcare naturally converge into a preventative medical model, as preventing diseases from happening to begin with leads to decreased medical bills, whereas remedial treatment leads to increased expenditures as the root cause of the associated disease is often left untreated. These preventative measures result in a ripple effect, exponentially decreasing the rate at which people get sick, and as a result further reducing required expenditure on healthcare.
In conclusion, high levels of funds is no replacement for proper allocation of said funds. Our findings are as follows:
- Healthcare sectors should adopt preventative measures for treatment as opposed to focusing on curing ailments as they arise
- Countries need to aim towards universal healthcare, and begin to adopt makeshift models until implementing such a system is feasible, or adopt it entirely if available funds allow it